Trauma – there is hope

Have you experienced overly stressful events that still haunt you and distress you?
You react, day after day, as if everything is happening again. The hormones from the stress spill over into your body – you sweat, your heart rate increases and you feel intense fear. Fear overwhelms everything. And you get so angry with everything and everybody!
You know it’s just a memory, but your brain and body react as if you are back to the original event.
Do you start your day already with a baseline of high stress?
Does this affect your life, prevent you from savouring the good times, and hold you back from pursuing your goals and having a regular and fulfilling life?
If this seems familiar, it is possible that you are suffering from PTS. You can complete this questionnaire – it will help you identify some of the symptoms and investigate if that is the case (Not a diagnostic).
Trying to treat trauma by getting people to ‘think differently’ (as in cognitive therapy) can be both awkward and ineffective because the problem is not due to how people think. People with PTSD know the event is in the past but feel like it is occurring now.
It is not possible to eliminate this emotion and what happens in your body just by using your thinking mind. You’ve tried, didn’t you?
Check the diagram beneath to understand the cycle of trauma.

How trauma can affect you
Don’t let Trauma define your life and limit your future. You can live a peaceful and fulfilling life no matter what happened to you in the past.
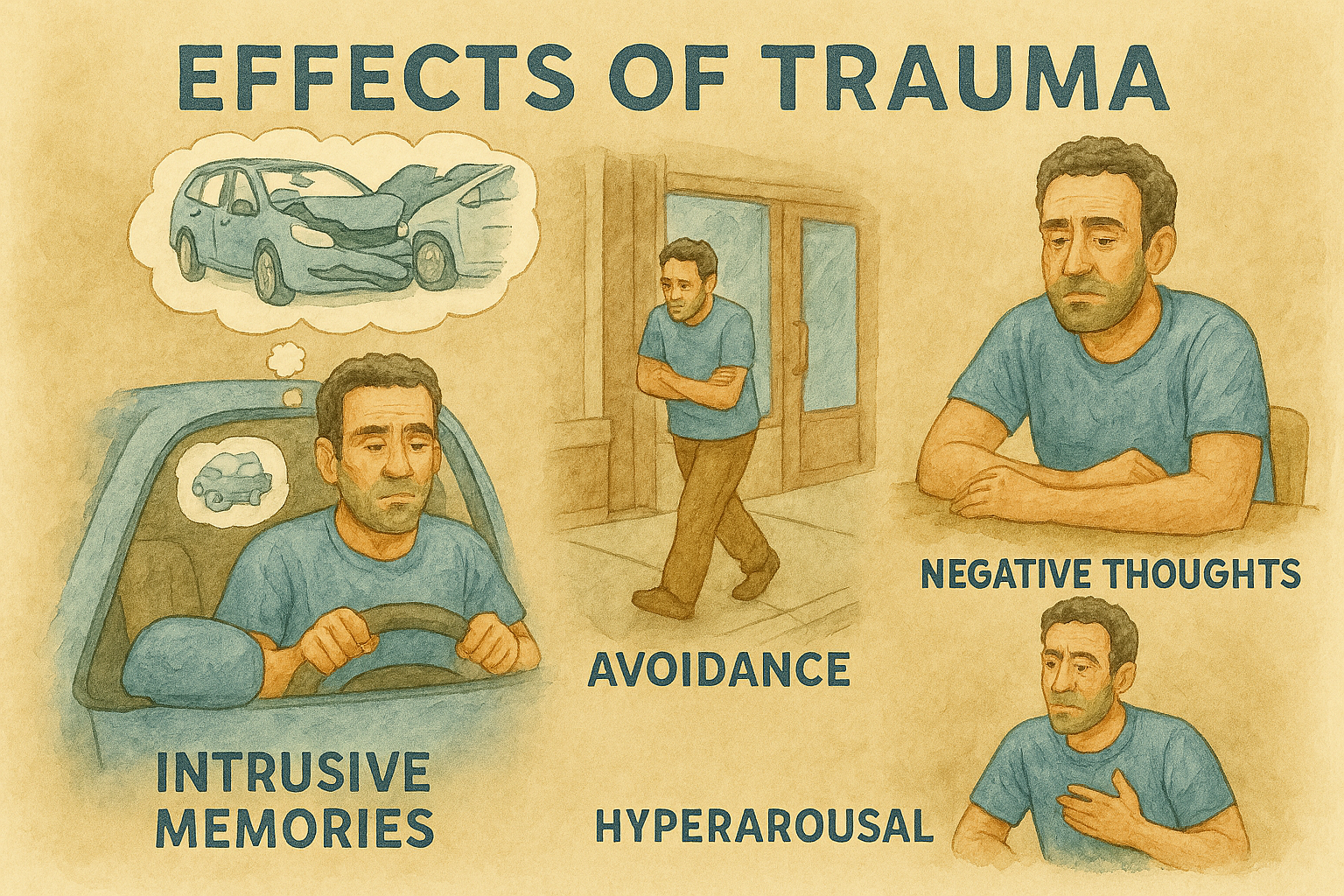
Traumatic memories can be behind your difficulties in relationships, anxiety, depression, phobias, addictions, weight gain, OCD, procrastination and other mental health conditions.
Trauma can result from shocking events like car crashes, war scenarios, natural disasters, etc.
It can also result from life intensely stressful events like a divorce, the death of a loved one, abusive relationships, bullying, and many other difficult situations.
Finally, complex trauma is present when we experience Childhood Adverse Experiences.
All of these have the same effect on us: difficulties in staying calm, gaining perspective and enjoying life, as well as distorted sleep patterns that leave us tired, unmotivated and fearful.
This changes the way our brain works, and conditions our interactions with other people, leading to problems in our relationships, jobs and general wellbeing.
Key Trauma Response Neurological Markers
- Heightened Amygdala Activation: Increased threat detection and emotional reactivity
- Reduced Hippocampal Function: Impaired memory integration and contextual processing
- Dysregulated Prefrontal Cortex: Compromised executive functioning and emotional regulation
- Elevated Cortisol and Stress Hormone Production: Persistent physiological arousal
The good news is that trauma can be reprocessed using specific Memory Reconsolidation Techniques.
We use a specialized technique called “the Rewind Technique“. It is a very gentle and relaxed way of memory reconsolidation. You don’t need to relive the traumatic event once and once again. You don’t even need to talk about it if that makes you uncomfortable.
You will leave therapy free from the weight of past events and ready to start again, afresh and resilient. When you resolve trauma everything else changes.
There is no pill that can cure this
What happens in your brain during traumatic experiences?
It is now known that trauma is a disorder of memory, it is not an anxiety disorder.
There is a “security guard” in your brain that is always scanning the environment, checking if it is safe to proceed. It is the amygdala. When the amygdala detects a threat to your survival, it signals the hypothalamus to release hormones that activate the fight-flight-freeze response. More specifically the pituitary gland releases endogenous opioids to help dull the pain and prompt the adrenal glands to release adrenaline, norepinephrine and cortisol. These hormones help you react quickly, give you strength to run or fight and numb the pain.
However, cortisol also inhibits activity in the hippocampus (memory) and pre-frontal cortex (rationality, creativity, solution focus, plant for the future). Cortisol is helping us to act instinctively, save energy and ensure all our attention and resources are used toward immediate survival. If cortisol didn’t do this, you may be tempted to pause and analyse the situation before acting, which could get you killed.
The freeze response

If the fight or flight response becomes exhausted, or if you are prevented from fight or flight, the brain activates a “freeze or submit-collapse” response through the parasympathetic nervous system (dorsal vagal nerve). This immobilizes your muscles and then they become limp. It can be frightening, but it is another way the mammalian brain learned to survive predatory threats. Our bodies “play dead” in hopes the predatory animal loses interest and move on. Opioids are released during the freeze response as internal pain killers and generally help us to dissociate or have little memory of the details of the event when it overwhelms our responses to cope.
Understanding the function of the dorsal vagal system explains why many people who suffered from PTSD had the experience of dissociating, collapsing or feeling completely paralyzed. People who have experienced this extreme dorsal vagal response often feel ashamed that they submitted, believing they were somehow complicit, weak or “broken” because they didn’t fight back.
You will feel some relief when you understand that the “submit and collapse response ” is activated unconsciously and is the body’s way of buffering from pain during a traumatic event.
During distressful experiences, the amygdala encodes all the sensory information associated with the event into what is called implicit memory. The implicit memory is a network of neurons that contains the felt, experimental part of a memory and has four components: 1) Emotional; 2) Perceptual; 3) Physical and 4) Procedural. These four components make up a mental model of the event that includes sensations, smells, sight, sounds, etc. Anytime your amygdala detects anything similar to the original traumatic event, it is primed to activate the same fight/flight or freeze response.
Under less extreme conditions, the thalamus, hippocampus and medial prefrontal cortex can stay online during the event and modify the learning in the amygdala by adding contextual detail to form an explicit memory. Explicit memory includes 1) the factual details of the event; 2) episodic memory – where the memory occurs in the timeline of your life and 3) autobiographical memory – the context and meaning of the event. This puts the memory in the right place and context and detaches the emotion from it.
What happens is that cortisol and opioids can interfere with the brain’s ability to form explicit memories during extreme stress events.
Thus, the sensory cues associated with the traumatic experience stay locked in implicit memory and fail to be integrated with the appropriate context and time.
Fortunately, there is something we can do. It has to do with a new discovery called “Memory Reconsolidation” which is changing the way we treat trauma.
Developmental trauma
Developmental trauma occurs when the traumatic stressors are chronic and happen during critical stages of development.
Abuse, neglect or chronic stress during childhood and/or adolescence reorganizes your brain and changes the way your brain functions.
Your brain is not trying to sabotage your life. It is simply responding to the way it was programmed to survive in a chaotic environment. Your brain needs to adapt to the onslaught of stress hormones flooding your neurons.
Neurons in the amygdala become enhanced for sensing danger. In the meanwhile, neurons in the pre-frontal cortex and in the hippocampus begin to atrophy, shrink and even die. The thalamus has difficulty in filtering out irrelevant stimuli, leading to sensory overload and feelings of overwhelming even from routine activities.
Numerous studies have shown that people who experience chronic abuse or neglect in childhood have problems
A) Identifying and regulating emotions
B) Controlling behavioural impulses
C) Focusing Attention
D) Making decisions and planning for the future
E) Getting along with themselves and others
F) Develop health problems such as obesity, heart disease, substance abuse, IBS, fibromyalgia and chronic pain.
Attachment styles
Our brains form an Internal Working Model for relationships based on the type of relationship (or lack of relationship) we had with early caregivers4. We call this out attachment styles5. We can have a secure or an insecure attachment style. Insecure attachment styles include an anxious attachment style, an avoidant attachment style and a disorganized attachment style.
New relationship experiences can also modify a person’s inherent attachment style. For example, someone who has a secure attachment style as a child could develop avoidant, anxious or disorganized traits after being in an abusive relationship. Likewise, an adult with an insecure attachment style could develop a more secure relationship behaviour upon experiencing a healthy, caring, long-term relationship with a partner, friend, or therapist.
But we all have the tendency to revert to the attachment style we formed as infants under times of extreme stress, or when forming a relationship with a new person.
If you wish to test your assessment style, please look here.
The antidote to developmental trauma is secure attachment
The neural pathways that shape our attachment schemas are stored in the non-verbal right hemisphere of the brain. It is not so much what the mother says to the baby that calms the baby down. It is the soft gaze of her eyes, the warm cradle of her harms and the soothing sound of her voice that treasures her baby that she is safe, wanted and loved. It is the right hemisphere that serves as a template for developing her sense of self, perception of others and emotional regulation skills.3
This correlates with Stephen Porges’s polyvagal theory, the three branches of our nervous system and the different states their activation produce and Daniel Siegel’s theory of interpersonal neurobiology.
This means that having someone in your life that is able to be an attuned presence and offer empathy, congruence and unconditional positive regard is essential to start to build new, more useful neuropathways in your brain.
Wounds from the violence weren’t nearly as devastating as the feeling that no one cared about them
C Armstrong, Rethinking Trauma
.
To recover from trauma, you need to:
- Experience a safe, trusting relationship with your therapist, so you feel comfortable and open to doing the necessary work (it is possible, even if that seems difficult for you right now – time and small steps)
- The support of someone who understands what is going on in your brain and how to send a message of safety to your limbic system
- Recognise the symptoms for what they are and learn to calm down when they arise
- Address any practical difficulties that are contributing to the raised stress levels
- Deal with the sadness, anger and worry thoughts and learn how to lift your mood
- Process the traumatic memory so that it no longer triggers distress
- Work towards meeting your emotional needs using your own resources.
- Apply the knowledge and coping skills to the current and future life stressors so you get free from limitations and able to design your life your way.
Effective Trauma Treatment
Neuroscience discoveries in the last 20 years have given us new insight and hope for healing trauma. We’ve learned how trauma disrupts healthy attachments and impacts the brain’s ability to regulate itself. We also learn the connection between the body and mind in terms of the huge influence trauma has in our body. But we also learned interventions that can help the brain repair and heal.
We also learn that trauma can have positive effects on people, too. Research has shown some people developed increased resilience, greater appreciation for life and an openness to new possibilities after trauma.
An effective trauma relief treatment must be able to generate both sufficient dissociation and sufficient calm/relaxation in the sufferer to allow the painful memory to be reconsolidated safely so that it can be moved from the emotional centre of the brain (amygdala) to the rational centre of the brain (neocortex), where it will be marked as a past, no longer threatening event.
Memory Reconsolidation and the Rewind Technique
In the 80s, PTSD was considered an anxiety disorder and people were treated with prolonged exposure therapy, so they would become desensitized. Unfortunately, exposure therapy not only runs the risk of retraumatizing and research shows that it only yields temporary results 1 .
By 2010 new research proved that PTSD is not an anxiety disorder, but a disorder of memory1. This brought new insight into trauma treatment.
The key is recalling the implicit memory while simultaneously evoking a new experience that changes the meaning of the memory and invalidates negative beliefs attached to the traumatic event. Neuroscientists call this new experience a “mismatch experience” because the new experience has to create a mismatch or prediction error that causes the emotional brain to update its prior learning.
Merely talking about the event to attempting to tame the emotional brain with verbal reasoning does not work.
There are several Memory Reconsolidation Techniques.
After studying and applying several of them, I found that the Rewind Technique is the most gentle, respectful and efficient way to help my clients.
The results continue to surprise me.
You will be in a calm state and with simple imagery, you will be able to put those memories in the right place and context.
You don’t need to revive the traumatic events once and once again. This technique allows you to look at the event (s) in a dissociative way, from an “observing-self” point of view. That changes the pattern matching in your brain.
And you don’t even need to disclose the event verbally to your therapist if you don’t feel like it.
It is possible to distance yourself from the event (s) and start remembering it like any other past memory
You have the resources that will help you to overcome trauma and live a peaceful life.
You just need some guidance
References
- LeDous, 2015
- DeBellis and Zisk, 2014
- Allan Schore, 2012
- Bolby, 1998
- Ainsworth, 2015




